by Nikos Mattheos, DDS, MASc, PhD
It was 2017 when I learned about the first autonomous robotic implant placement. Although a very exciting development, back then I thought this more of a “stunt” than a tool we will see soon entering clinics. Seven years down the road and robotics are being hailed as the next frontier—a technological revolution promising unprecedented precision, improved outcomes, and even the holy grail of fully automated dental procedures. But let’s take a step back and ask: how far have we truly come?
Will dental robotics ever become a mainstay rather than a niche curiosity?
Looking back in the (short) history
The year is 2017, a year that might be upheld in the future as a double-birthday among implant robotics enthusiasts. Neosis, a very young US-based company gets FDA approval for its implant robot Yomi. At the same year, a Chinese start-up places with great publicity the first robotic implant in China with their robot Yakebot. Both share the same dream of automated implant treatment, but the philosophies of their systems are rather different. Yomi is a system with low-level autonomy, what we would often call “level 1” or robotic assistance. This means that the surgeon needs to hold the handpiece while preparing the osteotomy, while the robotic arm only restricts it’s move to ensure accuracy. Yakebot on the other side is a task-autonomous robot or “level 2” meaning that the robotic arm can actually move independently to prepare the osteotomy and place the implant. Yomi is using a mechanical special positioning system, with a separate arm attached to the patient for real time positioning. Yakebot on the other hand is using an optical tracking system, which means that the robot tracks the real time position of the patient with cameras and optical trackers. The DNA of these two systems has proliferated to more than half a dozen implant robots that are commercially available today.
After their launch, both systems followed a similar path in their respective home countries. Yomi soon gathered more than 50,000 documented patient treatments, while Yakebot showed a similar trajectory, after it received Chinese FDA approval and became commercially available in 2021. Interestingly, the Chinese market grew fast with more than half a dozen robots entering the market soon after Yakebot, while Yomi has still to see a competitor in US (…but will finally have one next year!).
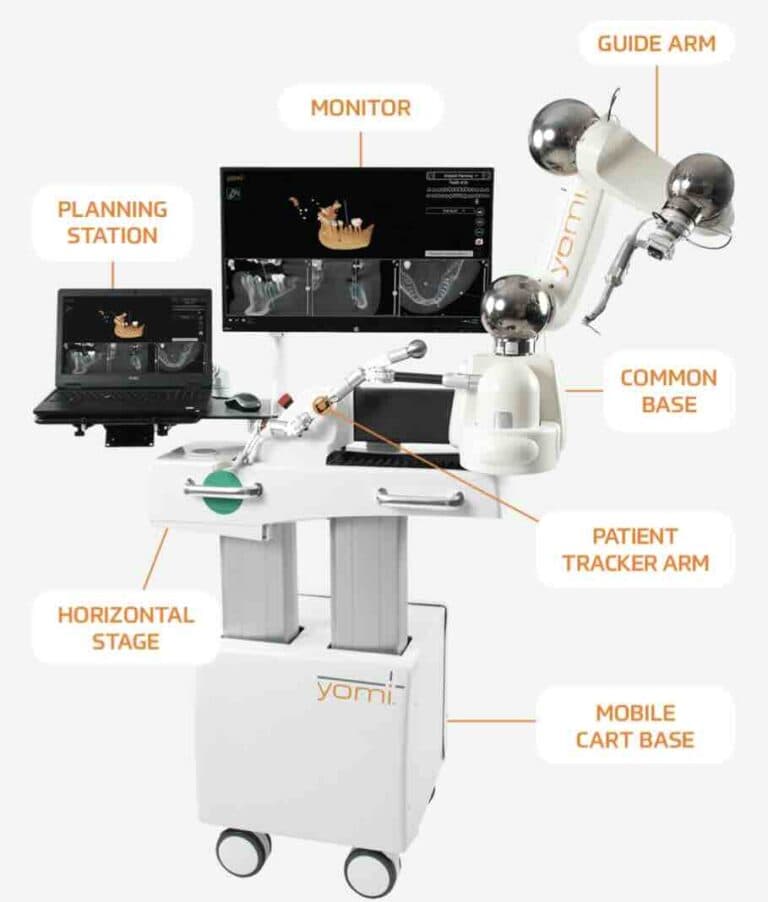

The promise of robotics
The human urge for automation is timeless and has been tempting our imagination since the beginning of history. From the novels of Isaac Asimov to modern day science fiction, a robot surgeon is a very appealing image indeed, But we now live the real-deal, it’s no longer sci-fi. Robotic surgery has already transformed fields of medicine like Urology and Orthopedics, bringing unprecedented minimal invasiveness and accuracy. Da Vinci, introduced in 2000 needed the best part of two decades to become widely adopted, but it is today the indisputable golden standard when it comes to soft tissue procedures like deep pelvic surgery. Likewise, Stryker and Zimmer robots have empowered flapless arthroscopy dramatically improving patients’ experience and literally cutting down recovery times by months in some cases.
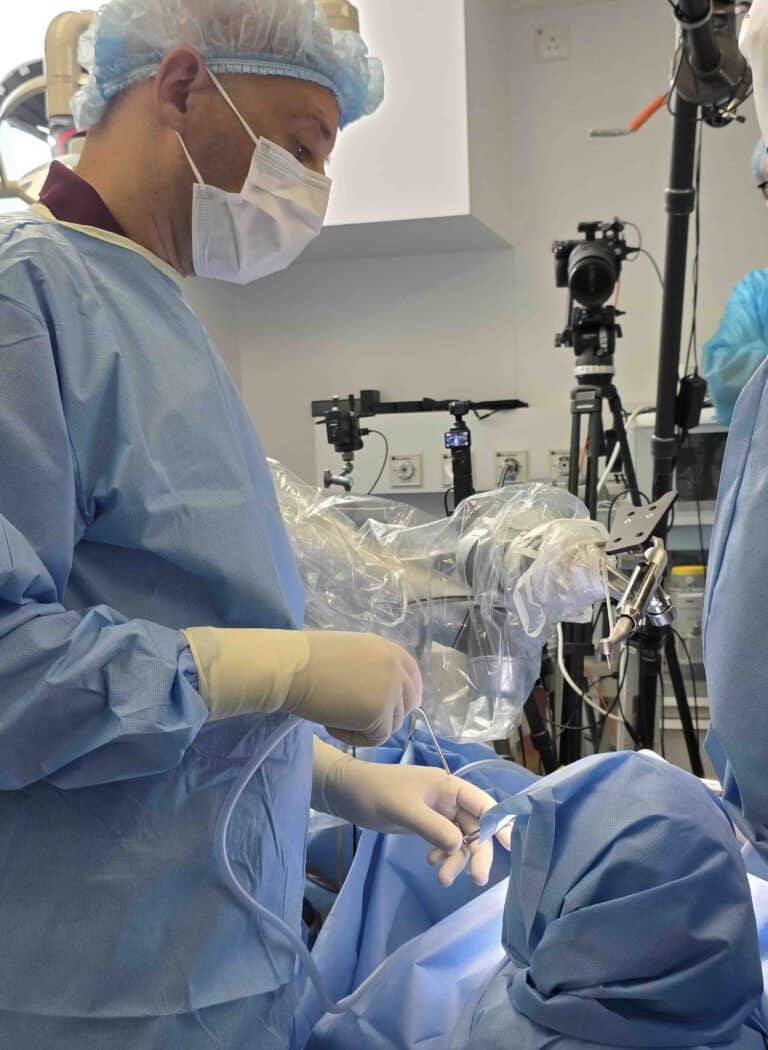
And now, robots are already placing implants - thousands of them and with staggering accuracy. They are not just “dynamic navigation with arms.” They’re a new species. But what do they really bring?
🤖 Getting Real About Robots
Looking at the marketing pitch of most implant robots, one word stands out: Accuracy. Indeed, robots have been placing implants with the highest accuracy, surpassing not only conventional non-guided surgery, but also human-operated static or dynamic guided surgery. How much exactly more, depends what you use to compare with. When we meta-analysed a large number of clinical trials, robots placed implants 0.7 mm and about 5.4 degrees more accurately than humans working freehand and 0.4 mm and about 2 degrees more accurate than humans using static or dynamic guided surgery. Statistically significant, but hard to interpret exactly what this additional accuracy means in clinical terms. There is no doubt that with a good digital treatment plan higher accuracy would mean better clinical outcomes, but where is the threshold and how much accuracy is enough? I guess the answer lies on the complexity of the treatment, as the “accuracy” tolerance differs from a single crown to a full arch.
Beyond accuracy however, the pitch of implant robotics gets a bit more vague.
Automation, is probably the second most used keyword, with the task autonomous robots able to conduct the osteotomy and place the implant with only human supervision. From a technological point of view, this is quite an achievement, with implant robots frog-leaping all established medical robots. Task autonomous implant robots like Yakebot and Remebot operate already in the level 2 of autonomy, while most medical robots are either fully controlled by the surgeon (level 0) or require his direct guidance (level 1). Automation has a major charm to most of us, watching a robotic arm conducting a highly precise surgical move all by itself is a thrilling emotion, at least for geeks like me. At the same time, the experience for the patient is not essentially different. On top of that, autonomous robotic placement is far slower and more complex at least for now. Moving the arm in and out in a case of multiple implants might significantly slow down the procedure. Thus, the small community of robotic users in implant dentistry is currently split, with many proponents of more automation (let’s break through to level 3 with the help of AI !), while others believe that the future lies in improving the effectiveness of surgeon-guided level 0 and 1 systems, like the US Yomi and the upcoming robot from X-nav. Such systems would be equally accurate and faster than task autonomous, but will require a constant “human touch”.
Unlike the medical robotics, which can get miniscule instruments through keyhole entries into otherwise unreachable areas of the body, implant placement with a robot follows the same procedure as with a human operator and offers little advantage in patient experience and healing outcomes, at least in conventional dental implant surgery. But maybe this is not the first place we should look.
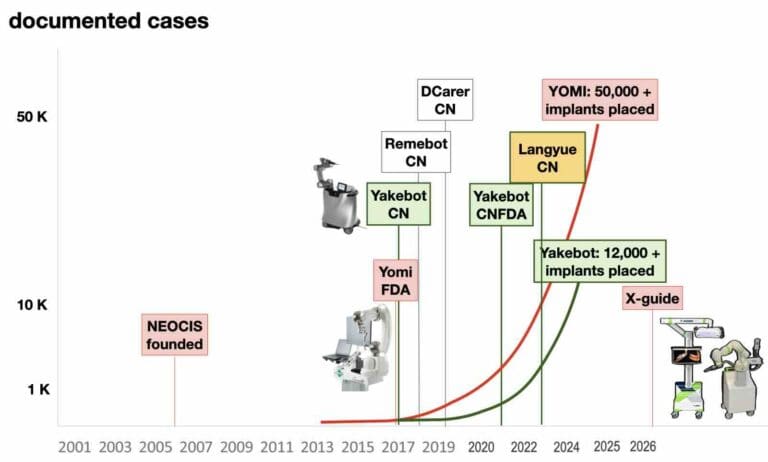
The Pathway to the "Miracle"
There is a certain repeated pattern in every technological “miracle”. We usually witness the “miracle” with excitement, but we often miss the path, which started from a “useless” tool, moved to a proof of principle and many staged of commercialization. Computers in the 60’s could do complex calculations much better than humans, but had the size of a one bedroom apartment, were expensive and incredibly complex to operate. This lead Thomas Watson -the chairman of IBM back then- to famously prophesised that “the world market for computers would be limited to just five machines”. Luckily for IBM, they did not give up. It took them the best part of 20 years till they managed to pack this computational power in a box the size of a large suitcase, but from this point onwards development was explosive. The IBM PC, the machine who changed forever our idea of a computer was launched only 6 years later and this is when most of us witnessed the “miracle”. (I actually couldn’t afford an IBM PC back then, so my miracle was much cheaper, but not any less exciting for sure).
Likewise the “miracle” of AI chatbots was founded in mathematic models developed already in the 60s. But without massive computational power and endless repositories of data, such a theoretical concept was a useless tool. Until gaming forced computational hardware to reach unprecedented performance (see NVDIA) and the World Wide Web became a massive repository of free content. Then suddenly it all fell in place and the miracle happened seemingly overnight (but it was not!)

There is a major principle with any technology: “make it first, then make it better”. Once a technology goes beyond the proof of principle, 3 things are for sure: It will get cheaper, it will get smaller and it will expand its scope to new areas.
The Breakthrough
Implant robotics is now in early commercialization and already a vibrant part of a wider $12 billion market of medical robotics. The brainpower and funds committed to research and development in this direction is unprecedented, as much as the cross fertilization between the different kinds, technologies and applications. Adding to this the explosive development of AI tools that can add functionality and open pathways in synergy with robotics and you have a massive ecosystems tuned for major breakthroughs. Enhanced software algorithms incorporating machine learning are beginning to allow semi-autonomous decision support. Haptic feedback systems and augmented reality interfaces promise are advancing rapidly. With half a dozen implant robots competing in China alone, we already see evidence of price reduction and miniaturization. Several different technologies are now put in competition: Optical tracking remains a major component, while some robots choose mechanical tracking arms which no longer require the presence of cameras. The battle between increased autonomy or human guidance is still ongoing with no definite winner, while the scope of robots is expanding to cover many other areas of oral surgery, restorative dentistry and more. Recent implant robots already double as dynamic navigation devices as well, while soon they will be able to perform many other procedures with additional software modules. The breakthrough in cost effectiveness, might actually come from the increased scope of indication or might come from the procedures of high complexity, like zygomatic implants. Based on some yet-unpublished data from a robot under development in US, robotic placement in zygomatic surgery can be both more accurate but also faster and less invasive than any other human operated surgery. This could be the breakthrough needed beyond accuracy, which would elevate these tools to the level of medical surgical robots and build further from there.
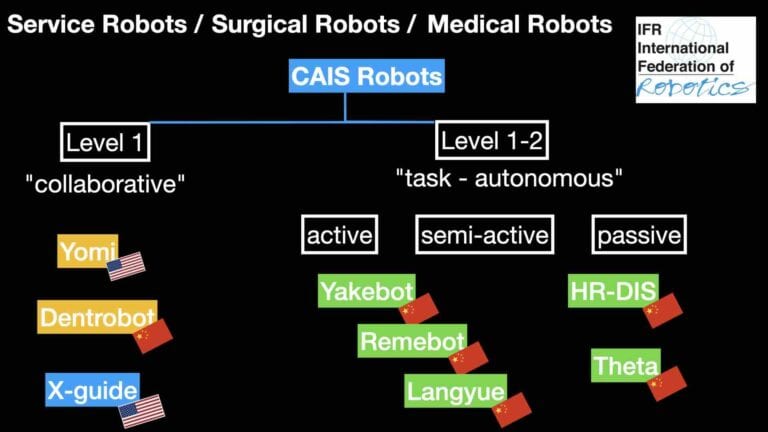
Currently available Computer Assisted Implant Surgery (CAIS) robots, as they fall under the Categories of Medical and Surgical robots of the IFR. Some in the collaborative level 0-1 of autonomy, while other in level 2 (task autonomy). Active, passive or semi-active refers to how the robotic arm is directed to the targeted area and whether the operator needs to define the path of insertion/withdrawal of the end effector (handpiece).
The Future
We are witnessing the birth of dental robotics, with implant dentistry being the spearhead. The Gini is out of the bottle and what we see is not a hype, but a technology trying to find its way to mainstream practice. Some will get burned on the way, but some will find it, just as sure as water find its way eventually to the sea. Technology alone will not make robotics the new standard. The human elements—effective training programs, seamless clinical protocols, patient education, and multidisciplinary collaboration—will shape its success. The complex biomechanics of the oral environment and patient experience demand that robotic systems integrate seamlessly with clinician judgment, not replace it.
As a sceptic, one can still find many barriers to point out, as this technology has yet to break into the cost-effectiveness zone and offer real solution to actual clinical problems.
As a visionary however, one cannot ignore the tectonic shifts that are currently transforming healthcare and surgery in particular. There is no way back. As a dentist, you can afford to be a late adopter. But for institutions, universities, companies and organisations which wish to stay in the forefront the time is now: it isn’t just about placing implants, It’s about redefining the frontiers of what care is possible.
Stay in touch and get the latest in Implant Dentistry:
Eager to learn more?
Master immediacy with dynamic navigation!
Learn all about immediate implants and test hands-on 4 different navigation systems in this unique 2-day intensive masterclass with Nikos Mattheos and Atiphan Pimkhakham in Bangkok!
25-26 April 2026
Dentopia, Bangkok

4 thoughts on “Robotics in Implant Dentistry: An Honest Pitch to Believers and Sceptics”
Yes, things are moving very fast indeed. If general surgery is a guide then robots will be in our practices soon! Then again I think implants is not a real beneficiary, maybe robots that do dental assisting, sterilising and organisation of instruments? scanning?
DaVinci is operated by a haptic control like a video game, or? Is this how the dental robots are also controlled?
Maybe the way practice of dentistry is moving from solo practice to multi-practice clinics and chains, will bring these robotics closer to the mainstream. Then again, does this benefit the patient in the end? I am not sure.
Robotics will dominate every aspect of social and professional activities soon I believe. Especially when Artificial Intelligence will blend with robotics, I think we will see many breakthroughs. Still placing implants is not where I would need a robot…anyone having a robot that can do periodontal treatments? scaling and polishing? that I would gladly delegate to a robot and I could keep it busy in my practice 🙂